
Background
Strokes are common – we all know of someone who has been affected by stroke disease. Every time I’m on call there are at least one or two people admitted to the hospital as an emergency with possible stroke. Just before the summer it happened to Mum.

Mum’s Story
What happened when you had your stroke?
It was 11th June 2019. I was at a meeting in a hilly part of Glasgow and when I came out I couldn’t walk properly. As I do have problems walking that didn’t take me too much by surprise. But when I tried to get in the car I had difficulty getting my leg in the door. I drove from there to my cousin’s new home. I thought there was something odd about their new carpet as my right foot seemed to be sticking to it.
We were looking through some old photographs later and I wrote the names of the people in them on the back. When I looked at them a few weeks later, I realised I’d written a lot of nonsense and not their names at all.
I drove home to Ayr and tried to make supper. When I tried to measure a spoonful of something I couldn’t shake off the excess. I tried to email and I couldn’t type and decided I must be really tired and went to bed.
Not long afterwards I wakened and my lips felt tingly. I remembered someone telling me that had happened to her when she had a stroke. When I tried to get up and my leg wouldn’t hold me we phoned for an ambulance.
What’s happened between then and now?
I remember going to hospital, but I can’t remember very much else for a few days. I do recall people saying I wasn’t speaking properly but thinking I definitely was. A friend who came to visit couldn’t work out what I was saying. I found it very strange as I could hear myself speaking exactly as I always do. I tried to draw a clock-face in hospital and it was a mess.
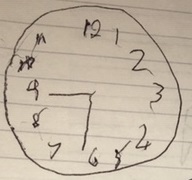
The doctor told me I’d had a small stroke and I thought that meant there wasn’t very much wrong. It was a small stroke and I’m not as badly affected as many people but I’ve discovered over the months there are lot of things that are more difficult to do that I didn’t realise until I tried to do them, things like drawing and painting which I’ve always liked doing.

I was dragging my foot behind me but that improved quite quickly. I realised what I needed to do and had to relearn it.
The hospital was wonderful although there were some silly design issues that made things more difficult. For example, the toilet roll was only on one side of the toilet, and as it was the side affected by the stroke I had to ask for help every time. I was in for ten days. I was ready to come home by then although I still wasn’t very mobile.

You’re a really busy person normally, when you came home it must have been a huge change to have to stop and sit back.
I didn’t have any energy so I had to.
Yes that’s something you mentioned a lot after you came home, even a few months later. Are you still seeing improvement, 6 months later?
Oh yes, absolutely.
How are you getting in on with your drawing and writing?

I have to concentrate really hard and think about what I’m drawing or writing. It still takes much longer than it used to but it’s definitely getting better. To start with I had to use my finger to follow what I was reading because every time I looked up I lost my place and had to start at the top of the page again. I still can’t glance down at a page and find where I was reading.
You’ve kept you’re self really active since you came home, haven’t you?
Yes, I go out a walk every day, whatever the weather – nearly! I use a delta frame outside. I still feel unsteady as I tend to go to right. I recently asked the physiotherapist about it and she advised me to look a little to the right and that really helped. I’ve discovered if I work out exactly what the problem is and ask the right question, I get the right answer. Everyone’s stroke is different and even professionals can’t read minds!

What did you find helped the most with your recovery?
The stroke nurse has been a huge help. She’s interested in the smallest thing and I feel I can ask her anything. Having her email address made me feel free to get in touch with her, for example, when I was having problems with my blood pressure being too high.
And the out-patient care I’ve had access to since I came home has helped enormously. The day hospital has been hugely helpful – the staff there have time to spend with individuals. The occupational therapists work out exactly what you need. It’s not one size fits all.
I’ve also been going to a support group and it’s been very useful. Over the course of the six weeks I saw a real difference in everyone in the group.

I’m a list maker and always have been. When I was in hospital I made lists of things I had to do for the physiotherapist, occupational therapist and speech therapist. Every night I made a to-do list for the next day with these things on it. I found the energy to do them because they were on the list and I knew they were crucial to my recovery.
Six months on I’m working at changing my mind-set. My to-do list is no longer a list of therapies but just life. So instead of writing “Physio” on my list, I write “Go for walk”. Instead of writing “Hand exercises”, I’ll write “Do jigsaw” or “Play Checkers”. This feels really important to me at this stage of my recovery.
I’ve also kept a journal which means I can look back and see how, with a vast amount of help and support from family and professionals, I’ve already come a long distance.

How do strokes happen?
A stroke happens when part of the brain is damaged because it’s starved of oxygen. This usually happens because a clot occurs in the blood vessel that supplies that area of the brain, or, more rarely, because there has been a bleed into part of the brain. The impact it has is depends on which part of the brain is affected. There are so many different types of strokes. They can result in loss of strength or feeling in the arms or legs or face, difficulties with vision, speech.
There are a number of different medical conditions that make your risk of stroke higher. Theses include hardening of the arteries to the brain, an irregular heart beat (atrial fibrillation) or previous heart attack, high blood pressure, diabetes, high alcohol intake, high cholesterol, obesity and smoking. People who have had a previous stroke or mini-stroke (TIA) in the past are also at higher risk.
Of course nothing can prevent a stroke completely but there is good evidence the following lifestyle changes can reduce risk:
- Dietary changes that are associated with lowering blood pressure, like reducing salt and saturated fat intake, and increasing intake of fruit vegetables and low fat dairy products.
- Increasing physical activity
- Reducing your weight if you are overweight or obese
- Keeping blood pressure well controlled
- Stopping smoking
- Avoiding heavy alcohol consumption
As well as this certain people at higher risk may benefit from aspirin or cholesterol lowering tablet therapy. Particular conditions like high blood pressure and atrial fibrillation (an irregular heart beat) may also require specific medication.
How do you recognise the symptoms of a stroke?

Remember the FAST acronym – it helps people identify stroke symptoms.
FACE: Has their face fallen on one side? Can they smile?
ARMS: Can they raise both arms and keep them there?
SPEECH: Is their speech slurred?
TIME to call 999 if you see any one of those symptoms.
Izzy
©AYOSC 2019
2 replies to "Mum’s Stroke"
Great article that others can learn from (not least the loo roll!) and lovely thing to do for your Mum.
Aw thanks! I’m glad you enjoyed it, Izzy